Florida’s Revolutionary Pilot Program Offers Immediate Support to Overdose Survivors
Florida’s pilot of the Coordinated Opioid Recovery program offers those who overdose a better, faster route to recovery.
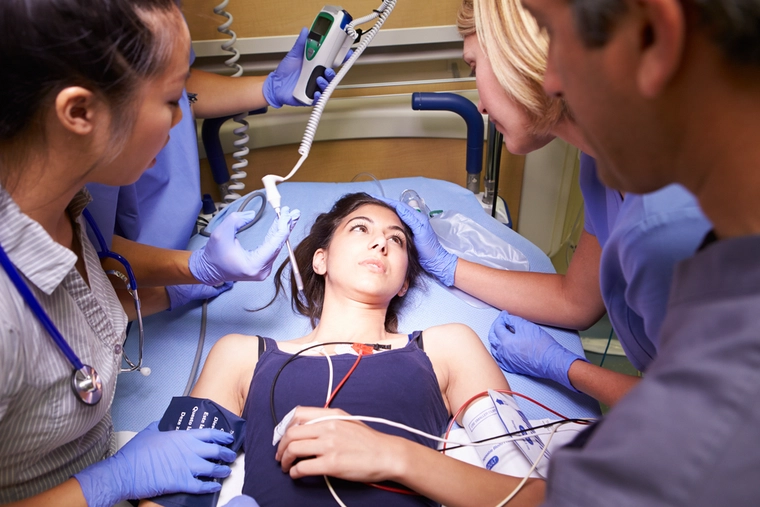
In 2022, Florida Governor Ron DeSantis announced a pilot program that takes immediate and effective action to save those who have suffered non-fatal overdoses. This program increases the speed at which a person who just overdosed can access drug rehabilitation services so they can escape this kind of danger in the future.
Without a program like this, what far too often happens is that when a person overdoses, they are revived at the site of the overdose and then taken to the emergency room for further treatment. Some people refuse further care and walk out. Others may stay for a while, but then, when they are discharged, they return to the same life and drug use as before. Very few ask for help getting into a drug rehabilitation program.
These people’s lives are at risk every single day unless they can get effective assistance to break the cycle of addiction. A look at the situations faced by those who overdose, by the first responders who save them and emergency room staff reveals the importance of a program of this type.
A Chaotic ER Situation
When a person overdoses on an opioid, the deadly effects of the drug can be reversed with the opioid antidote naloxone, often brand-named Narcan. It must be given quickly enough after the overdose, however. First responders that are able to administer naloxone soon enough will watch the person snap back to consciousness in less than a minute.
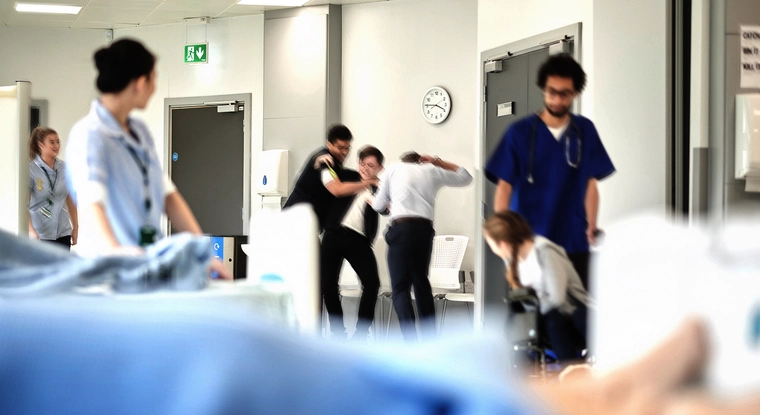
In some cases, the disoriented person coming out of drug-induced unconsciousness will react violently, as this law enforcement officer described:
I have had a few people get legitimately upset with you because you ruined their high. I try to stay close because some people do come out swinging. I had one grab a medic and I had to kick them in the face.
One study of reactions seen after administering naloxone noted that about one-third of those revived responded with anger. Some people who are given too much naloxone will experience instant withdrawal sickness and pain that is precipitated by the antidote1. It is very difficult to administer the right amount of naloxone unless a first responder receives sufficient training.
The reactions of those being revived can make an emergency room chaotic and somewhat dangerous. The burden of having to revive more than one person every night also increased ER chaos, as well as first responder and ER staff burnout.
Officers Required by Law to Take an Overdosing Person to the ER
In some jurisdictions, officers are required to take the individual to a hospital for further treatment and monitoring. The other option is taking the person to jail. One officer described this choice:
It’s not an “If”—it’s a “You’re going to the hospital.” If they won’t go, we will force them to go under immediate detention…. If they don’t go to the hospital and get more Narcan they will overdose again. We use that as a justification of making them go.2
Another officer described the role they must play when out in the field:
We don’t let people walk away that have overdosed. They will go to the hospital whether it’s on their own or through immediate detention. Because once you walk off, that Narcan can wear off and you will drop off.2
These two officers’ statements describe the intensely dangerous situation these opioid-addicted people are living in.

Narcan’s Life-Saving Effects Are Short-Lived
One problem with bringing a person back from an overdose is that the effects of some opioids last longer than the antidotal effects of Narcan. Therefore, the benefits of Narcan may wear off while the stupefying effect of an opioid is still coursing through their body. That person may go right back into an overdose when the Narcan wears off. For that reason, some force or coercion is applied to get overdosing individuals to stay in the hospital until they are completely out of danger.
A police officer in New Orleans accurately described the shortcomings of bringing a person to an ER and making no more effort than that to help them.
We’re constantly bringing people to the ER while knowing full well that the ER is not the answer for them. They need a lot more help than the 20 minutes we’re able to give them.3
https://www.nola.com/entertainment_life/health_fitness/overdose-what-happens-when-the-medics-arrive/article_d40955ac-f8bb-559b-ae91-f453db959d32.html Overdose: What happens when the medics arrive 2019
Doctors have had few tools to get these individuals any real help. They could refer the person to a support group or counselor, but it was up to the patient to make the connection. This pilot program offers a better solution.
Florida’s Pilot Program to Provide Immediate Help
Florida’s pilot is called CORE—Coordinated Opioid Recovery (CORE). In this pilot, which is running in a dozen locations, emergency medical technicians take a person revived from an overdose to a special facility. If needed, they will bypass multiple conventional emergency facilities on the way there.
Once they arrive, the person rescued from an overdose will see a practitioner with specialized training. When it’s been determined that the individual is stabilized and out of danger, they will be offered immediate services to help them escape the addicted lifestyle they have been living. If they accept, they will be walked into a drug rehab program without delay.4
This immediate help is a far better solution than simply sending this addicted person back out to the streets. ER Doctors often report seeing the same person again in the same month, the same weeks, or even the same night. One person who overdosed and was saved twice in one night returned a few months later—sober—to thank the first responders who saved him. Unfortunately, his story is not that rare.5
Social Support Is Also Needed

Another vital type of support that will be offered as part of this pilot program is social support services that address housing, food insecurity, and employment. Many people who are addicted have already lost everything by the time they suffer a near-fatal overdose. Without support for housing, food, and employment, they may not have a chance to re-integrate into society as they work to overcome their addiction.6
This pilot was launched in Palm Beach County for almost two years and then was expanded to Brevard, Clay, Duval, Escambia, Gulf, Marion, Pasco, and Volusia counties in its first phase. Its second phase will include Citrus, Duval, Flagler, Manatee, and Pinellas counties.
Sources:
-
“Perspectives from law enforcement officers who respond to overdose calls for service and administer naloxone.” Health and Justice Journal, 2022. HJJ ↩︎
-
“Factors Associated with Withdrawal Symptoms and Anger Among People Resuscitated from an Opioid Overdose by Take-home Naloxone.” National Library of Medicine, 2022. NLM ↩︎ ↩︎
-
“Overdose: What happens when the medics arrive.” Nola.com, 2019. nola.com ↩︎
-
“New opioid recovery pilot program coming to 12 Florida counties.” State of Reform, 2022. State of Reform ↩︎
-
“He overdosed twice in 24 hours, then came back to thank his rescuers.” Palm Beach Post, 2017. Palm Beach Post ↩︎
-
“Ending Addiction in Florida.” Florida Government, 2022. Florida Government ↩︎






 ®
®